Colorectal Cancer
What is Colorectal Cancer?
Because colon and rectal cancers occur from the same type of cell and have many similarities, they are often referred to collectively as “colorectal cancer”.
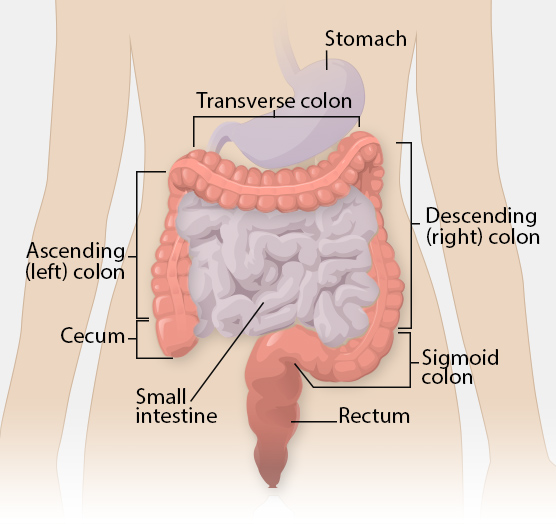
Our gastrointestinal system digests food and absorbs nutrients. Oesophagus, abdomen, small intestine, and large intestine make up the digestive method. The large intestine begins with the colon, which is around 5 feet long, and ends in the rectum and anal canal. Caecum and ascending colon, transverse colon, descending colon, and sigmoid colon is four parts of the colon.
The colonic wall has four layers of tissue. Cancer happens when cells in the body develop uncontrolled. Colon cancer starts in the innermost layer, the mucus-producing cells that line the colon. Most colorectal cancers beings as small mounds of flesh called polyps. Over time, some of these polyps grow into colon cancer. It then advances through the colonic wall and to the adjacent lymph nodes and spreads across the body
Signs and Symptoms
Colorectal cancer may cause one or more of these symptoms:
- A change in bowel habits, such as diarrhoea, constipation, or narrowing of the stool, that lasts for more than a few days.
- A feeling that you need to have a bowel movement that is not relieved by doing so.
- Rectal bleeding.
- Blood in the stool, which may cause the stool to look dark.
- Cramping or abdominal (belly) pain.
- Weakness and fatigue.
- Unintended weight loss.
Most of these problems are more often caused by conditions other than colorectal cancer, such as infection, haemorrhoids, irritable bowel syndrome, or inflammatory bowel disease. Still, if you have any of these problems, it’s important to see your doctor right away so the cause can be found and treated, if needed
Risk factors
Like most types of cancer, colorectal cancer is normally in older people. More than 80% of colorectal tumors (8 in 10) are identified in people over 60.
The exact cause of colorectal cancer is unknown. But several things called risk factors can improve the chances of growing it. Having one or more risk factors doesn’t mean you will get cancer.
- Older age
- Western diet (a diet rich in fat, red meat, and prepared meat; low fibre diet)
- History of colorectal polyps (adenomatous polyp, large polyps, and multiple polyps)
- Family records of colorectal cancer (1 in 3 people who improve colorectal cancer have family members who had it)
- Previous history of colorectal cancer (if you have been treated for colorectal cancer earlier)
- Inflammatory bowel disease of the colon; ulcerative colitis and Crohn’s disease (the risk of cancer increases with duration and severity).
- Diabetes
- Obesity
- Physical inactivity
- Smoking and alcoholism
Treatment
If it′s detected early enough, treatment can cure colorectal cancer and stop it from coming back. Unluckily, however, a complete cure is not always possible and there is sometimes a risk that cancer could recur at a later stage.
In advanced cases that cannot be eliminated by surgery, a cure is highly unlikely. However, symptoms can be managed and the extent of cancer can be slowed using a combination of surgery, chemotherapy, radiotherapy, and biological treatments where appropriate.
Treatment plans are created to meet the unique needs of each person with cancer.
Treatment decisions for colorectal cancer are based on:
- Stage
- Type of cancer (colon or rectal)
- Location of the tumour
- Whether the cancer has recurred or spread
- The person′s overall health
Surgery for Colon Cancer
If colon cancer is at a very initial stage, it may be possible to extract just a small piece of the lining of the colon wall. This is known as local excision.
If cancer develops into muscles surrounding the colon, it will usually be required to remove an entire section of your colon. Eliminating some of the colons is known as a colectomy.
There are two ways a colectomy can be performed:
- An open colectomy – where the surgeon creates a large hole in your abdomen and removes a section of your colon. Types of Colon Surgeries are as under :
- Removal of a polyp (polypectomy)
- A polyp is not cancer, but there may be cancer cells within a polyp. If polyps are discovered during colonoscopy or sigmoidoscopy, they are surgically extracted and checked for cancer cells.
- Elimination of tumors in the mucosa layer of the colon (local excision or endoscopic mucosal resection)
- Elimination of part of the colon (hemicolectomy, partial bowel resection)
- Elimination of all of the colon (colectomy, total bowel resection)
- Extraction of all of the colon, rectum and pelvic organs (pelvic exenteration)
- Extraction of colon cancer that has spread to the liver or lung (metastases)
- A laparoscopic (‘keyhole′) colectomy – where the surgeon makes several small holes in your abdomen and uses special instruments guided by a camera to remove a section of colon
During surgery, nearby lymph nodes are also removed. It is common to join the ends of the bowel mutually after bowel cancer surgery, but very hardly this is not possible and a stoma (see below) is needed.
Both open and laparoscopic colectomies are thought to be equivalently useful in eliminating cancer and have similar risks of complications. Laparoscopic colectomies, however, have the advantage of a faster healing time and less post-operative pain and this is becoming the routine way of doing most of these operations.